What to expect during IUD insertion
An intrauterine device or IUD is a small T-shaped device that a doctor or nurse can implant into the uterus to prevent pregnancy.
It is among the most effective forms of reversible birth control with a failure rate of less than 1%. The insertion is a minor medical procedure that only takes a few minutes.
Research has shown that while women report insertion experiences that range from painless to extremely painful, the procedure is usually less painful than they expected.
In this article, learn about what to expect during an IUD insertion. We also cover the side effects and recovery.
Preparation
Before getting an IUD, a person can speak to their doctor about which type is best for them. IUDs come in two forms:
- The copper IUD: This version of the device kills sperm, preventing it from fertilizing an egg.
- The hormonal IUD: This type of device releases progestin, which is very similar to progesterone, a hormone the body manufactures itself.
Progestin can prevent ovulation, which means there is no egg for the sperm to fertilize. It also thickens cervical mucus, making it more difficult for sperm to travel to the egg if the body does ovulate.
Hormonal IUDs may help with some premenstrual and hormonal symptoms, such as heavy bleeding or period cramps.
Copper IUDs do not offer any benefit other than contraception, so doctors do not usually recommend them for people who already experience heavy bleeding or severe cramps during menstruation.
IUDs are safe for most people to use. However, those who are allergic to copper should not use a copper IUD.
An IUD can prevent unwanted pregnancy but cannot protect against sexually transmitted infections (STIs).
People should not use an IUD if they have had any of the following:
- abnormal vaginal bleeding
- vaginal or cervical cancer
- a recent pelvic infection or STI
Women who are pregnant or want to become pregnant should not get an IUD, although it is safe to get an IUD soon after childbirth.
In some people, progestin increases the risk of blood clots in the leg or high blood pressure, so it is vital to tell the doctor about any cardiovascular or other health problems.
Many people worry about pain during an IUD insertion. However, a recent study found that women’s self-reported pain, following IUD insertion, was significantly lower than the pain they expected to experience.
Some research suggests that anxiety before the procedure can make insertion feel more painful. Working with an empathetic doctor or nurse, who is willing to take time to discuss the procedure and offer reassurance, may help.
A person may wish to consider asking a doctor what previous experience they have of inserting IUDs. Similarly, they can tell the doctor if they are feeling nervous about what is going to happen.
Some people report that taking over-the-counter (OTC) pain medication, such as ibuprofen, before the procedure helps reduce pain afterward.
During the procedure
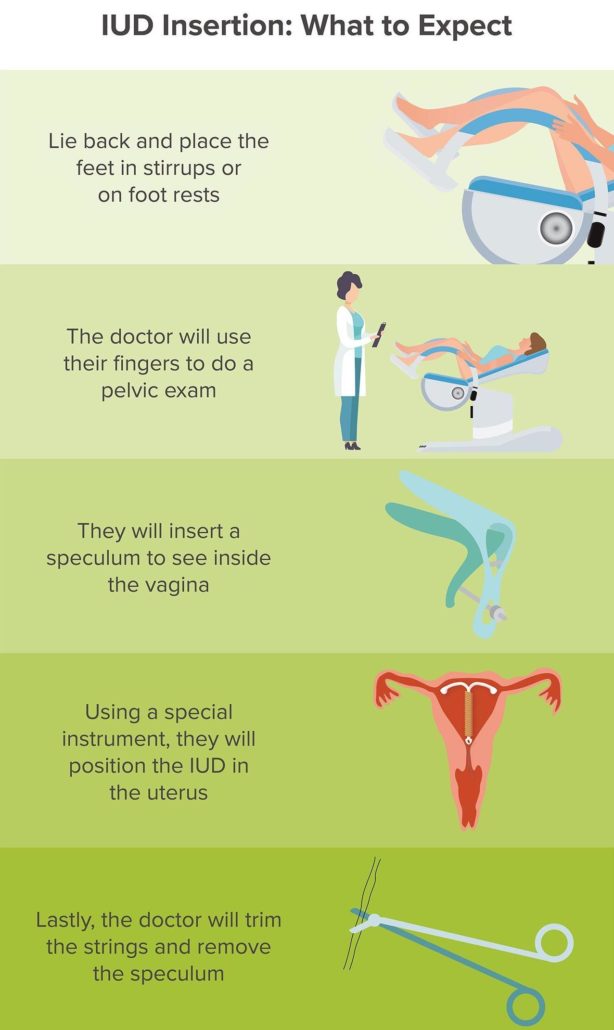
During the procedure, a person will remove their undergarments and other clothing from the waist down. They will then lie on their back, usually with their legs in stirrups. A doctor or nurse will offer a sheet to cover the thighs to help a person feel more comfortable and less exposed.
The doctor will first conduct a pelvic exam using the fingers, then cleanse the vagina and base of the cervix with an antiseptic solution.
They will then insert a speculum into the vagina to separate the walls, enabling them to see better. Using a small instrument, they will insert the IUD into the uterus through a small opening in the cervix.
Some people experience cramping similar to or sometimes more intense than menstrual cramps. If the pain feels unusual or unbearable, the person must tell the doctor. The whole process usually takes only a few minutes.
After the insertion
Some people feel dizzy or faint after an IUD insertion, so it can be a good idea to have someone accompany them for the journey home.
It is usually safe to return to work or school right away. However, if a person is feeling intense pain or cramping, they may wish to rest for a day.
Following insertion of an IUD, it is normal to notice some spotting. According to Planned Parenthood, spotting can last up to 3–6 months.
The individual should ask the doctor how long to wait before having unprotected sex. IUDs cannot prevent STIs, so it is important to practice safer sex with new or untested partners.
Aftercare
One of the main benefits of an IUD is that it requires no special care. In the days following insertion, it is common to experience some cramping and spotting. OTC medication can help reduce these symptoms. Any pain should disappear in a few days.
The IUD attaches to a string that enables a doctor or nurse to remove the device. Some women can feel the string with their fingers. It is best to leave it alone. The string is not dangerous but pulling it could move or even remove the IUD.
If the string causes irritation or if a partner can feel the string during sex, a person can ask a doctor to trim it.
In rare cases, an IUD can come out on its own. If this happens, it is possible for the person to become pregnant. Anyone whose IUD has fallen out should call a doctor and not have unprotected sex.
Side effects
Copper and hormonal IUDs can cause side effects, although these usually resolve after a few months.
Side effects of the hormonal IUD can include:
- spotting
- missed periods or no periods
- headaches
- bloating
- nausea
- breast tenderness
- changes in breast size
- mood swings
- depression
- low libido
- weight gain
Not everyone experiences side effects or all of the above that doctors associate with IUDs.
Side effects of the copper IUD can include:
- pain and cramping
- a backache
- long and heavy periods
- irregular periods
- spotting
Complications with an IUD are relatively rare, but can include:
- the IUD falling out
- problems associated with the hormonal IUD, such as changes in blood pressure or blood clotting.
- an ectopic pregnancy, or pregnancy outside of the uterus
- infection following insertion
- pelvic inflammatory disease, if a person already has an infection before the IUD insertion
- damage to the uterus
People with a history of cardiovascular disease, those who smoke, and those who are over 35 years old are more likely to have complications from a hormonal IUD.
It is a myth that IUDs can travel to other areas of the body, such as the brain or lungs.
Removal
IUDs can prevent pregnancy for 3 to 12 years and sometimes longer. It is possible to remove the IUD at any time.
During removal, a nurse or doctor will ask a person to lie on their back and put their feet in stirrups.
They will insert a speculum to open the vagina and then gently tug on the IUD string. This causes the IUD to fold and pass through the cervix. A person may experience cramping during removal, but the procedure only takes a few minutes.
Sometimes the IUD is harder to remove. If this happens, a doctor might use smaller instruments to take it out. Very rarely, if an IUD is stuck, a person may require surgery to remove it.
When to see a doctor
People should see a doctor if the following symptoms appear shortly after IUD insertion:
- a fever above 101°F
- chills
- intense or unbearable cramping
- strong, sharp pain in the stomach
- very heavy bleeding
Call a doctor for these symptoms at any time after insertion:
- a missed period with a copper IUD
- a positive home pregnancy test
- an IUD that falls out or seems to be coming through the cervix
Summary
An IUD is an excellent option for people who want long-term birth control without remembering to take pills, receive injections, or use condoms.
As with any birth control, IUDs offer both benefits and risks. If a person is unsure about whether it is the right choice for them, they can speak to a doctor to discuss their concerns.
The IUD insertion can be uncomfortable or painful for some people, but the pain usually passes. It may also cause some side effects as the body gets used to the new device.
It is best to speak with a doctor about any side effects if these interfere with a person’s overall well-being or quality of life.
 Request An Appointment
Request An Appointment COVID-19 Vaccine
COVID-19 Vaccine



